Hey readers —
We’re back with another company deep dive, where we look at how teams are actually building and deploying AI in healthcare.
This time, we’re covering Lumeris and Tom, its AI-powered ‘Primary Care as a Service’ platform. Rather than building another point solution, Lumeris is taking a systems-level approach, embedding AI directly into primary care workflows to expand access, support clinicians, and help health systems serve more patients.
Inside: why the real constraint in primary care is people, not tools, how Tom operates as an AI team member rather than software, and what it takes to deliver “best next actions” at population scale.
Let’s dive in. 👇
Read time: 7 minutes
TOGETHER WITH LUMERIS
Company Deep Dive: Lumeris
Perspectives from the people building the future of health AI…

We sat down with Jean-Claude Saghbini, Chief Technology Officer & President of Technology Services at Lumeris, to unpack how the company is approaching one of healthcare’s biggest structural challenges: access to primary care.
With more than 20 years of healthcare experience, Lumeris has spent over a decade working with health systems to improve outcomes and reduce costs through primary care transformation. With Tom, the company is extending that model by introducing an AI-powered primary care team member that operates alongside clinicians, helping expand capacity, coordinate care, and drive action across large patient populations.
Jean-Claude shared how Tom functions as an end-to-end AI operating system for primary care, why AI should be used to serve more patients rather than replace existing workflows, and what it takes to deploy this kind of infrastructure inside real health systems.
Let’s start from the top. What’s your background, and how do you describe Lumeris today?
I’m an engineer by background and have spent my entire career in technology, with the last 20 years focused on healthcare. I started in an early RFID company building devices and cloud infrastructure for health systems and medical device manufacturers, which was later acquired by Cardinal Health. I went on to run that business and later served as CTO at Wolters Kluwer Health.
I joined Lumeris about five years ago because it brought me closer to the front lines of care delivery, even though it’s not a provider itself. It’s a transformational model focused on improving outcomes and lowering costs, which aligned with what I wanted to work on.
Lumeris is built on the premise that primary care is the most efficient point to transform healthcare. By improving primary care, we can meaningfully improve outcomes and reduce total cost of care.
Over time, we’ve built both technology and operational infrastructure to help health systems transform primary care. That includes working across value-based care models and supporting millions of patients through partnerships with health systems nationwide.
What led to the creation of Tom?
We had already built a lot of infrastructure to support operators working with health systems, but we were still limited in our ability to take action at scale.
When large language models became viable in 2022, it created an opportunity to reason across large patient populations and actually drive actions, not just generate insights. At the same time, we stepped back and realized the bigger issue wasn’t just optimizing care, it was access.
There are roughly 100 million Americans who either don’t have access to primary care or receive suboptimal care, and we’re facing a shortage of nearly 90,000 primary care physicians. That’s the problem Tom was designed to address.
What is Tom and ‘Ask Tom’, in simple terms?
Tom is both a platform and a participant in care delivery.
It’s a Primary Care as a Service platform that uses AI to help deliver care at scale, but it also functions as an always-on AI member of the care team. It works alongside physicians and staff, engaging with patients directly and supporting care delivery under the direction of the primary care team. Tom reviews patient panels, makes proactive patient outreach, surfaces best next actions, and executes them, all while improving access to care and reducing administrative burdens.
We recently introduced Ask Tom, which is an analytics capability within the Tom platform designed to give health system leaders and clinicians access to enterprise data and performance insights across clinical and operational domains.
Ask Tom is a natural language interface that creates a comprehensive view by pulling from integrated clinical, claims, pharmacy and social determinants data within Tom.
Instead of relying on analysts to generate reports, users can directly ask questions and understand what’s happening across their patient populations, including trends, issues, and performance. It builds on the same data and infrastructure that powers the rest of the platform.
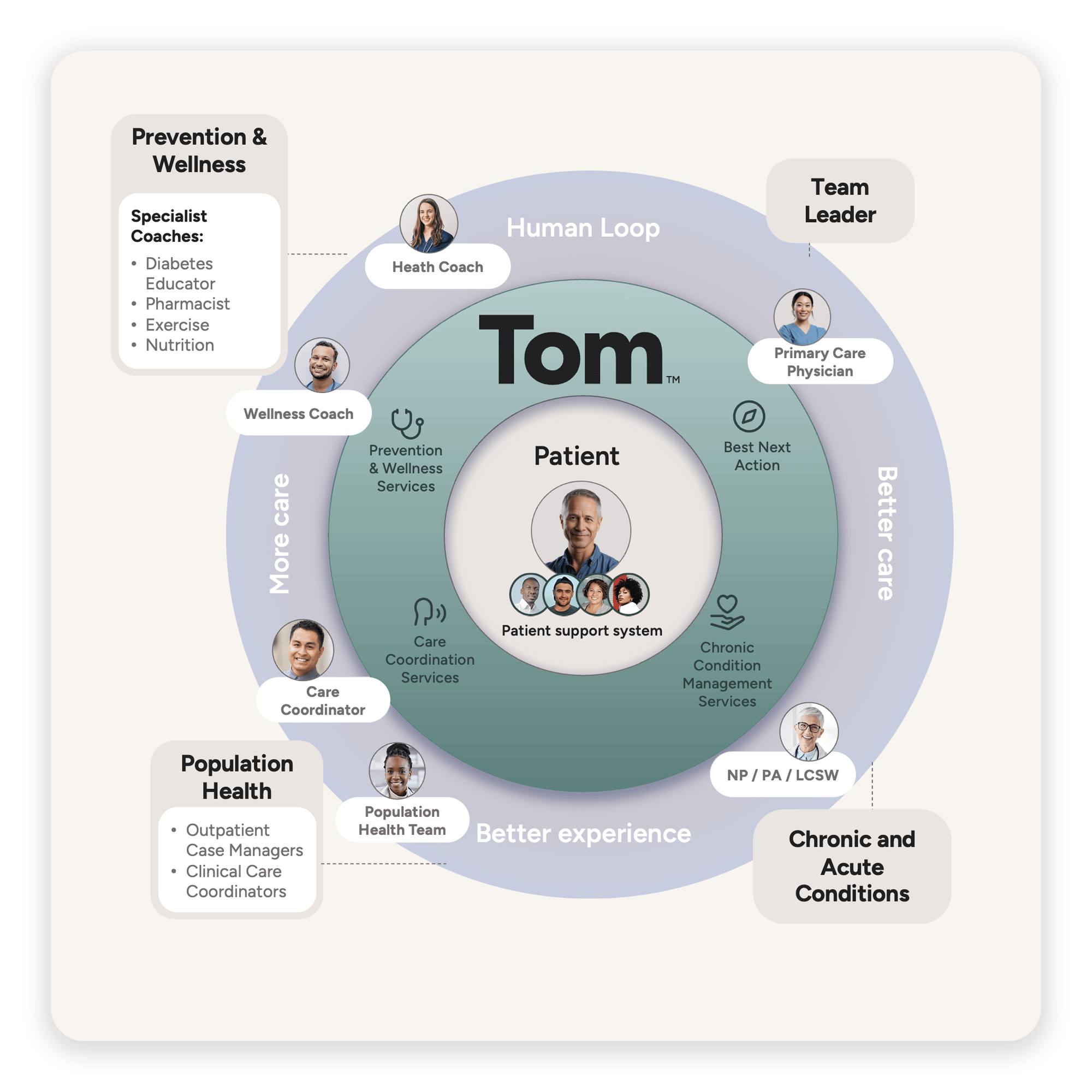
What core problem are you solving in primary care?
The real constraint isn’t tools, it’s people.
As I mentioned earlier, nearly 100 million US adults lack primary care today, and we’re heading toward a shortage of almost 90,000 physicians. At the same time, Americans over 65 will soon outnumber those under 18, accelerating rates of chronic disease, cancer, cognitive decline, and behavioral health needs. Together, these forces are driving a steep rise in demand for coordinated, longitudinal care.
Health systems have built infrastructure and have patients who need care, but they don’t have enough clinicians or hours in the day to meet that demand. Tom is designed to act as additional capacity within the care team, helping bridge that gap rather than adding another layer of software.
You describe Tom as an “operating system” for primary care. What does that mean in practice?
Delivering primary care as a service requires an end-to-end system, not a collection of point solutions.
That means ingesting and normalizing data from multiple sources, building a complete patient view, generating insights, and determining what actions should be taken. It also requires the ability to execute those actions, whether that’s outreach, education, scheduling, or care coordination.
On top of that, you need clinical workflow integration, decision support, analytics, governance, and safety mechanisms. All of those components working together is what we mean by an operating system.
Who is the primary user of Tom, and how does it fit into clinical workflows?
The primary user is the primary care team.
Tom acts as an additional team member rather than a replacement. It expands the team’s capacity while keeping clinicians in control. Most of the care team continues to work within the EHR, and Tom’s outputs are surfaced directly there.
Tom fits into existing workflows rather than require clinicians to adopt new systems. We think of it less as software deployment and more like onboarding a new team member that adapts to how the organization operates.
At the same time, Tom interacts directly with patients in many cases by extending support beyond the visit with personalized outreach, education, and reminders. Tom listens to the patient, remembers, and responds based on each patient’s history, risks, and needs. This helps to ensure that no one falls through the cracks. Tom reaches out by phone or text meeting patients where they are, with empathy and consistency.
How does Tom determine the “best next action” for a patient?
It starts with aggregating and analyzing a wide range of patient data.
We use a multi-agent system to reason across that data and determine what actions will move a patient toward a better health outcome. That could include outreach, care coordination, or other interventions.
Because this is a complex problem, we’ve also built internal probes to understand how the system is reasoning and to monitor performance as it evolves.
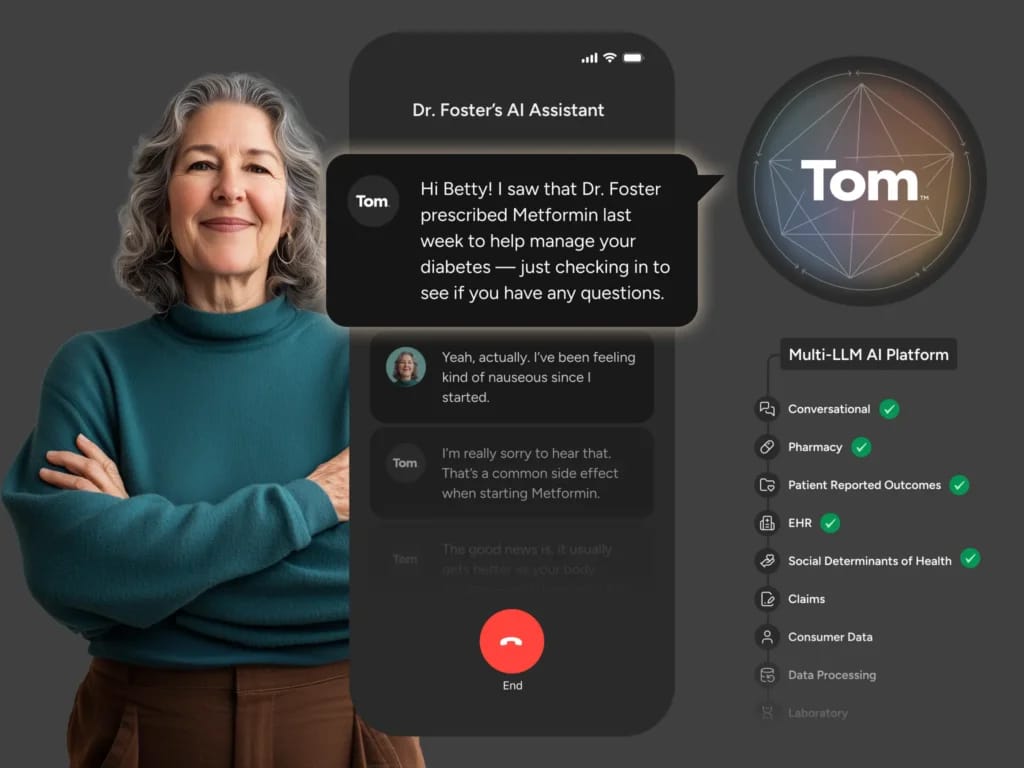
What does the technology stack look like under the hood?
Data is the foundation. We’ve spent years building pipelines that integrate with dozens of EHRs and payer systems, and we’ve designed them to handle the inconsistencies and failures that are common in healthcare data.
We also incorporate additional datasets, including consumer data, to better understand patients. Once aggregated, we standardize everything using frameworks like FHIR to create a unified record.
On the AI side, we use multiple models and approaches depending on the use case. Our current foundation is built around our partnership with Google and Gemini, but we don’t rely on a single model. We apply different methodologies depending on what we’re trying to achieve.
How do you approach safety, guardrails, and evals?
We think about it in three phases: before, during, and after development.
Before development, we focus on governance, trust, and compliance. During development, we use tools to test whether the system is following guidelines and staying within defined guardrails.
After deployment, those monitoring tools continue running in production. They track behavior, detect drift, and support escalation when needed. We use a combination of internally built tools and third-party solutions to manage testing and security.
What does implementation look like, and who is the ideal customer? How do you think about ROI?
Implementation typically takes a few months, usually around two to three months for an enterprise deployment. That includes data integration, workflow alignment, and onboarding Tom into the organization. It’s not a single switch. It’s more like introducing a new team member whose capabilities expand over time.
The ideal customer is a health system that has strong demand for primary care but lacks the capacity to meet it. These organizations have already invested in infrastructure and want to expand access to more patients.
From an ROI perspective, the primary benefit comes from serving a larger population. Health systems generate downstream revenue from additional services, patients get access to care they otherwise wouldn’t receive, and the system benefits from reduced total cost of care.
Where is this going, and what do you think the industry gets wrong about AI?
Our roadmap focuses on expanding Tom’s capabilities, deepening the clinical services it can support, and staying adaptable as AI continues to evolve.
More broadly, I think the industry often focuses too much on automation and cost reduction. The bigger opportunity is solving problems we haven’t been able to address, especially access.
In healthcare, the goal shouldn’t be to serve the same patients with fewer people. It should be to serve more patients with the same workforce. If we only focus on efficiency, we miss the larger impact AI can have.

Healthcare AI Guy Summary
What stood out, what’s tricky, and why it matters…
Lumeris is taking a different angle on healthcare AI by going after one of the system’s core constraints: primary care capacity. Instead of building another point solution or workflow layer, they’re positioning Tom as an AI-native operating system that sits inside the care team and helps drive day-to-day decisions and actions.
Primary care in the US is under real strain, with roughly 100 million adults lacking access and a projected shortage of close to 90,000 physicians in the coming decade. At the same time, demand is rising as the population ages and chronic disease becomes more prevalent. Soon, there will be more Americans over 65 than under 18.
Lumeris’ bet is that AI can do more than make workflows incrementally better. Tom is designed to work across patient data, identify the best next action, and in many cases help carry it out, whether that’s outreach, scheduling, or care coordination. The goal is to take non-clinical work off the care team’s plate in a meaningful way, while keeping clinicians in control so they can see and care for the patients that need support
What stands out is the full-stack mindset. Tom depends on data aggregation, reasoning, orchestration, and execution all working together. It feels closer to an embedded teammate than a standalone tool, extending what primary care teams can realistically handle. Founded in 2010 and backed by investors like Deerfield and Kleiner Perkins, Lumeris has the operating experience and footprint to take a real swing at this.
What stood out
Primary care as the constraint, not the workflow: Most companies focus on making clinicians more efficient within existing workflows. Lumeris is trying to expand the number of patients the system can actually serve. That perspective shows up clearly in how the product is designed and where it fits.
AI as an additional care team member: Tom is meant to participate in care delivery, not just support it from the sidelines. It helps decide what should happen next and can move parts of that forward, which is a step beyond typical copilots and dashboards.
Full-stack operating system approach: Delivering something like “Primary Care as a Service” requires more than good models. It depends on data pipelines, orchestration, workflow integration, and execution all working together. It’s a heavier lift, but also harder to replicate if done well.
‘Best next action’ as the core idea: Rather than focusing on documentation or single workflows, Tom is centered around deciding what should happen next for each patient. That’s a higher-order problem and aligns more directly with outcomes.
Built on real operating experience: This isn’t a net-new startup approach. Lumeris is layering AI onto years of experience in managing risk, which shows up in how they think about incentives, deployment, and day-to-day realities.
What’s tricky
Working across fragmented systems: Primary care data is messy and is distributed in a lot of places: EHRs, payers, and external sources. Pulling it together into something reliable and up to date is hard, and everything else depends on getting that right.
Expanding capacity without overwhelming systems: If Tom successfully increases access and patient volume, health systems still need to absorb that demand across downstream services. Improving access at the front door can create pressure elsewhere.
Balancing automation and comfort: Moving from suggestions to action introduces new questions around trust. Even with clinicians in the loop, there’s a line that needs to be managed carefully as more tasks get automated.
Final thoughts
Lumeris is going after a problem that sits at the center of the healthcare system. Their approach stands out because it focuses on not only optimizing existing or creating new workflows but also increasing the system’s ability to deliver care.
The broader vision is where primary care becomes more continuous, proactive, and less tied to individual visits, which lines up with where the system likely needs to go.
If Tom can consistently identify the right actions and help move them forward in a way that clinicians are comfortable with, it could change how primary care teams operate. But getting there requires more than frontier AI, it’s an operational challenge as much as a technical one.
This is less about adding another tool and more about reshaping how care gets delivered. If it works, it could meaningfully expand access to primary care. It’s one of the more important problems in healthcare, and Lumeris has both the operating experience and scale to make real progress here.

This issue is presented in partnership with the featured company.
That’s it for this deep dive friends! Back to reading — I’ll see you next Tuesday.
Stay classy,
PS. I write this newsletter for you. So if you have any suggestions or questions, feel free to reply to this email and let me know
How was this week's newsletter? Tap your choice below👇


